Inflammation is a physiological process that is considered normal, being a response that promotes the healing of injured tissues.
When infected by bacteria, viruses, or any kind of microorganisms, the body reacts by producing an inflammatory response that is protective in nature. White blood cells are produced to counter the invaders. White blood cells produce chemicals that fight the invention. A network of many cells achieves this feat – the cells are namely neutrophils, monocytes, mast cells, and lymphocytes.
So when is inflammation bad? It happens when the immune system produces inflammatory responses even when there are no foreign invaders. People with autoimmune diseases also experience this. Their immune system produces unneeded inflammatory responses causing damage to normal tissues.
Inflammation is also a bad thing when the body’s immune system is weak and is constantly infected by pathogens producing frequent inflammatory responses of the immune system. Inflammation can be short-term or long-term. Short-term inflammation is acute inflammation. Long-term inflammation is chronic inflammation.
Types of Inflammation
Acute inflammation – Damages to tissue due to a traumatic injury, invasion of microbes, and exposure to noxious chemicals – all of this causes acute inflammation.
Chronic inflammation – Long-term inflammation lasts for a bigger duration than acute inflammation. Untreated acute inflammation leads to chronic inflammation. It can also depend on the body’s ability to tide over the damage. The longer the repair and recovery process, the longer is the presence of inflammation in the body, which can eventually lead to chronic inflammation.
Causes of inflammation
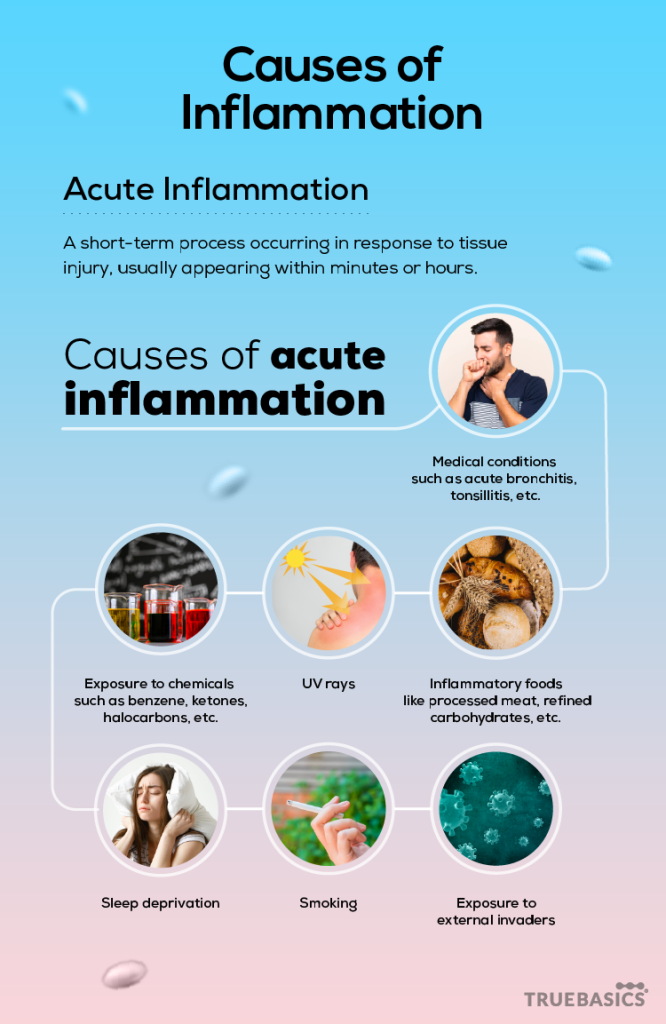
- Causes of acute inflammation:
Acute inflammation can be caused by immediate reasons such as a knee bruise (injuries), or a sprained ankle. The blood vessels will dilate, leading to redness and swelling, which usually subsides with time and medication/treatment for the underlying cause.
Other causes of acute inflammation include:
Diseases – Medical conditions such as acute bronchitis, tonsillitis, etc can induce an inflammatory response in the body.
UV rays – Ultraviolet rays cause an acute inflammatory response in the skin by inducing the release of proinflammatory cytokines.
Inflammatory foods – Processed meat, refined carbohydrates, vegetables, seed oils, etc can induce inflammation in a region depending on the underlying condition.
Exposure to chemicals – Chemicals such as benzene, ketones, halocarbons, etc can leave the exposed regions in an inflammatory state.
Smoking – Nicotine present in the cigarettes activates some white blood cells called neutrophils that cause inflammation in the body.
Exposure to external invaders – Inflammation is the body’s response to an injury or a pathogen or infection.
Sleep deprivation – Loss of even a single night’s sleep can lead to a cellular pathway that causes inflammatory responses in the body tissues.
- Causes of chronic inflammation:
Acute inflammation-causing infectious microorganisms are not removed from the body. This is because of the body’s inability to remove the infection and also the infectious microorganisms able to override the defense of the host.
When chemical irritants or foreign materials are inside the body via inhalation of the subject, it is removed by breaking down the irritants with enzymes or by way of phagocytosis – which is the ingestion of harmful foreign bodies by phagocytes. If both these processes are unable to remove the foreign materials, chronic inflammation manifests in the body.
Immune system disorders can sometimes cause the immune system to be hyperactive. A hyperactive immune system triggers inflammatory responses that attack normal healthy tissues and damage them.
Chronic inflammation isn’t always a progression of acute inflammation. It can manifest as a standalone response too. As an example, medical conditions such as arthritis and tuberculosis can cause chronic inflammation without the person necessarily having a history of acute inflammation.
Other causes of chronic inflammation:
Chronic stress – Studies have shown that chronic stress can alter the gene activity of immune cells, causing them to be ready to fight trauma even when there isn’t any.
Alcoholism – Overconsumption of alcohol on a regular basis leads to the overproduction of reactive oxygen species, known for their ability to stimulate a key inflammation transcription factor.
Obesity – Obesity can cause low-grade chronic inflammation. Fat is basically adipose tissue, and this tissue stores energy in the form of triglycerides, and produces molecules called adipocytokines which induce a chronic inflammatory response in the body.
Chronic inflammation in different regions of the body can lead to different serious medical conditions:
- Dermatitis – The inflammation of the skin. It can be caused due to use of certain cosmetics, detergent products, exposure to metallic compounds that have nickel, etc.
- Bronchitis – When the bronchial airways become inflamed, the inside of the tubes fills up with mucus. Mucus is a fluid secreted by the linings of tissues. The function of mucus is to trap bacteria, smoke, or dust apart from protecting and moisturizing the tissue surface. Excessive mucus build-up is characteristic of an inflammatory response. The mucus build-up in the bronchial airways causes breathing difficulty.
- Otitis media – It is caused by the inflammation of the Eustachian tube. This tube can become inflamed due to flu infection, smoke allergy, etc. The Eustachian tube is essentially a connecting passageway from the middle ear to the throat.

Symptoms of inflammation
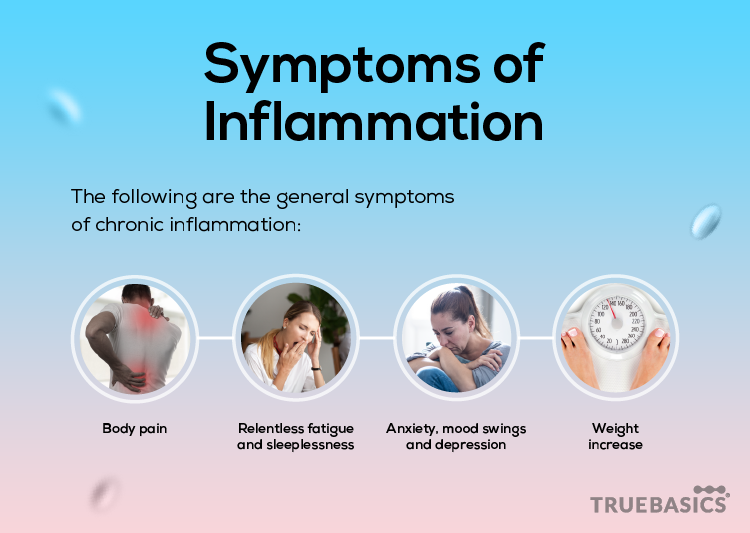
The following are the general symptoms of chronic inflammation:
Body pain – Body pain is a result of over-sensitized nerve fibers. Prostaglandin receptors regulate the pain. Body pain is generally reduced by inhibiting the synthesis of prostaglandin.
Relentless fatigue and sleeplessness – It has been studied that cytokines cause fatigue and insomnia during inflammation. Cytokines are secreted by the immune system during an inflammatory response. Biological agents that suppress cytokines are known to reduce fatigue and insomnia.
Anxiety, mood swings, and depression – Although inflammation does not have a direct correlation with depression, the onset of inflammation and associated physiological changes can cause depression. Medication administered to counter chronic inflammation, specifically, cytokine inhibitors have been studied to affect cortical and subcortical areas of the brain.
Weight increase – Due to a reduction in metabolic rate, obesity can manifest in those with chronic inflammation.
The following are the general symptoms of inflammation that are flu-like:
- Feverishness – It includes chills, feeling of fatigue, energy loss. There is a rise in temperature in the entire body resulting from the site of infection.
- Headache – Sinus cavities become inflamed leading to headaches.
- Decreased appetite – It is the body’s response to prevent the virus from growing further.
What happens when inflammation occurs?
When inflammation occurs, you feel a sensation of heat in the affected region. The most common outcome is redness, itchiness, irritability, and swelling of the area. If it’s joint inflammation, then there can be a loss of function or loss of movement of the joint.
Being a biological reply of the immune system to trigger a response because of pathogenic infection, inflammation can happen anywhere. It could be in any of the vital organs as well. Inflammation can happen in the kidney, lungs, brain, heart, intestine, pancreas. etc.
Depending on the extent of the injury or infection, more white cells may be present at the site. Given that white blood cells are producing inflammatory substances, the presence of the secretions causes irritation around the joint. Over a period of time, the joint lining swells. The continuous swelling can cause damage to the cartilage – which cushion the bone’s end parts. Cartilage damage can cause joint pain because the bone movement is rigid and will lack smoothness. Loss of cartilage means that movement of bones causes more friction – causing discomfort while walking, moving, sitting, or standing.
Being a response that initiates a healing process by removing stimuli causing the inflammation, the inflammatory response interacts at the cellular and molecular level.
What are the lasting implications of inflammation?
If left untreated, inflammation can become chronic. Most people are of the false impression that inflammation is only external in nature – characterized by swelling, reddishness, pain, etc. But in reality, inflammation can be the cause of major diseases such as diabetes, heart disease, etc if left untreated.
Over a period of time, chronic inflammation can cause long-term tissue damage. Health organs, cells, and tissues can get damaged in the process. At the severest level, DNA damage can cause irreversible damage that can lead to fatal consequences.
Possible Mitigatory Actions/Preventative Measures
Anti-inflammatory foods –
Eating or including anti-inflammatory foods as part of one’s diet can reduce inflammation. There are foods that cause inflammation and foods that reduce inflammation. Some examples of inflammation-causing foods are red meat, refined carbohydrates, margarine, and fried foods.
Some examples of anti-inflammatory foods are olive oil, fatty fish, Omega-3 fatty acids (which release specialized pro-resolving mediators (SPMs) which control the blood vessel inflammation), blueberries, strawberries, oranges, tomatoes, etc.
Lifestyle changes –
- Exercising – According to a recent study, regular exercise can help boost the immune system, developing anti-inflammatory properties.
- Balanced Diet – Consuming a balanced diet with fatty fish/fish oil, green leafy vegetables, nuts, olive oil, etc can mitigate inflammation effects as they are anti-inflammatory foods.
- Stress Management – Prolonged stress can lead to hyper physiological levels of cortisol, and inflammation is the body’s response to this condition.
Medication –
Anti-inflammatory drugs work by reducing the work of neutrophils – which increase inflammatory response by infiltrating tissue cells. Neutrophils are bacteria-fighting cells in the body. Created in the bone marrow, neutrophils are white blood cells and work by traveling to the site of the infection and neutralizing the bacterial infection.
- Corticosteroids – They are a category of steroids that lower inflammation by decreasing the immune system’s activity.
- NSAIDs (Nonsteroidal anti-inflammatory drugs) – It works by blocking the manufacture of prostaglandins, which in turn reduces redness, irritability, and swelling. Prostaglandins are similar to hormones. They perform physiological functions such as relaxation of muscle, blood vessel dilation/constriction, blood pressure control, and inflammation reduction.
- DMARDs – Expanded as disease-modifying antirheumatic drugs, this works by reducing the onset of rheumatoid arthritis.
- Biologic medication – It falls in the category of biologics. They are genetically modified protein compounds. The medicines work by targeting specific immune system areas that are causing the inflammatory response.
- Antimalarial drugs – A common drug in this category is Hydroxychloroquine. It is used generally for rheumatoid arthritis. Upon obtaining treatment, you will feel immediate relief. Swelling, joint pain, and stiffness reduces drastically.
NSAIDS, Biologics, and many other categories of medication work by inhibiting COX-1 and COX-2 – which are enzymes. These enzymes are responsible for manufacturing the compounds that trigger the inflammatory response. By inhibiting these enzymes, symptomatic relief is immediately attained. It is especially helpful for those who have chronic inflammation.
A combination of medication, diet, lifestyle changes, and exercise can control acute inflammation. If left uncontrolled, tissue injury happens over a period of time and causes major diseases or terminal diseases.
Food sources to reduce inflammation
Macronutrients combined with omega-6/3 fatty acids can reduce needless inflammatory responses.
Fruits – strawberries, raspberries, blueberries, blackberries.
Fatty fish – Fatty fish are rich in Omega-3 fatty acids. Salmon, mackerel, sardines, herring, and anchovies.
Broccoli – Being a cruciferous vegetable, Broccoli has antioxidants that reduce cytokine synthesis, and reduce inflammation.
Bell pepper – High in Vitamin C, the acids, namely, sinapic and ferulic in peppers can reduce inflammation.

Conclusion
With proper diet, sleep, lifestyle changes, medication, and moderate exercise, inflammation can be controlled, and even cured. Chronic inflammatory conditions must be immediately attended to. If you have chronic inflammation, consider expert medical treatment because if left untreated, it can cause terminal illnesses.
Sources:
- “Risk Factors: Chronic Inflammation – National Cancer Institute.” 29 Apr. 2015, https://www.cancer.gov/about-cancer/causes-prevention/risk/chronic-inflammation. Accessed 23 Mar. 2020.
- “Inflammatory responses and inflammation-associated … – NCBI.” 14 Dec. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5805548/. Accessed 23 Mar. 2020.
- Chronic Inflammation. (2020, Feb 14). Retrieved March 25, 2020, from https://www.ncbi.nlm.nih.gov: https://www.ncbi.nlm.nih.gov/books/NBK493173/
- “Transglutaminase 2 mediates UV-induced skin … – Nature.” 26 Oct. 2017, https://www.nature.com/articles/cddis2017550. Accessed 6 Apr. 2020.
- “Gastritis – MedicineNet.” https://www.medicinenet.com/gastritis/article.htm. Accessed 6 Apr. 2020.
- “Chemical-induced inflammation and inflammatory … – NCBI.” https://www.ncbi.nlm.nih.gov/pubmed/8972163. Accessed 6 Apr. 2020.
- “Missing link between smoking and inflammation identified ….” 31 Oct. 2016, https://www.sciencedaily.com/releases/2016/10/161031110809.htm. Accessed 6 Apr. 2020.
- “Loss Of Sleep, Even For A Single Night, Increases ….” 4 Sep. 2008, https://www.sciencedaily.com/releases/2008/09/080902075211.htm. Accessed 6 Apr. 2020.
- What Are Autoimmune Disorders? (n.d.). Retrieved March 25, 2020, from https://www.webmd.com: https://www.webmd.com/a-to-z-guides/autoimmune-diseases
- “Inflammation: The Common Pathway of Stress-Related … – NCBI.” 20 Jun. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5476783/. Accessed 6 Apr. 2020.
- “Alcohol, inflammation, and gut-liver-brain interactions … – NCBI.” 21 Mar. 2010, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2842521/. Accessed 6 Apr. 2020.
- “Low-grade inflammation and its relation to obesity and chronic ….” https://www.sciencedirect.com/science/article/pii/S0185106316300737. Accessed 6 Apr. 2020.
- “Understanding Eczema | Eczema Exposed.” https://www.eczemaexposed.com/understanding-eczema. Accessed 6 Apr. 2020.
- “Eustachian Tube Dysfunction – FamilyDoctor.org.” 8 Jan. 2020, https://familydoctor.org/condition/eustachian-tube-dysfunction/. Accessed 23 Mar. 2020.
- Inflammatory Pain. (n.d.). Retrieved March 25, 2020, from https://www.sciencedirect.com/: https://www.sciencedirect.com/topics/medicine-and-dentistry/inflammatory-pain
- Fatigue in chronic inflammation – a link to pain pathways. (2015, Oct 5). Retrieved March 25, 2020, from https://www.ncbi.nlm.nih.gov: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4593220/
- Andrew H. Miller, M. (2018, April 30). Five Things to Know About Inflammation and Depression. Retrieved March 25, 2020, from https://www.psychiatrictimes.com/special-reports/five-things-know-about-inflammation-and-depression: https://www.psychiatrictimes.com
- “Mysterious Fevers and Pain? You May Have ….” 25 Oct. 2018, https://health.clevelandclinic.org/mysterious-fevers-and-pain-you-may-have-autoinflammatory-disease/. Accessed 6 Apr. 2020.
- “What Your Flu Headache is Telling You – National Headache ….” 26 Feb. 2018, https://headaches.org/2018/02/26/flu-headache-telling/. Accessed 6 Apr. 2020.
- “Decreased Appetite: Symptoms, Signs, Causes & Treatment.” https://www.medicinenet.com/decreased_appetite/symptoms.htm. Accessed 6 Apr. 2020.
- “Inflammation – Medical News Today.” 24 Nov. 2017, https://www.medicalnewstoday.com/articles/248423. Accessed 23 Mar. 2020.
- Foods that fight inflammation. (2018, Nov 7). Retrieved March 25, 2020, from https://www.health.harvard.edu: https://www.health.harvard.edu/staying-healthy/foods-that-fight-inflammation
- “Anti-Inflammatory Diet: Foods That Reduce … – WebMD.” https://www.webmd.com/diet/anti-inflammatory-diet-road-to-good-health. Accessed 5 Apr. 2020.
- “How fish oil might reduce inflammation – Medical News Today.” 16 Dec. 2019, https://www.medicalnewstoday.com/articles/327322. Accessed 5 Apr. 2020.
- “Just 20 minutes of exercise enough to reduce inflammation ….” 16 Jan. 2017, https://www.medicalnewstoday.com/articles/315255. Accessed 5 Apr. 2020.
- “Anti-Inflammatory Diet: Foods That Reduce … – WebMD.” https://www.webmd.com/diet/anti-inflammatory-diet-road-to-good-health. Accessed 5 Apr. 2020.
- “How fish oil might reduce inflammation – Medical News Today.” 16 Dec. 2019, https://www.medicalnewstoday.com/articles/327322. Accessed 5 Apr. 2020.
- “Inflammation: The Common Pathway of Stress-Related … – NCBI.” 20 Jun. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5476783/. Accessed 5 Apr. 2020.
- “Neutropenia: Causes, Symptoms, and Treatment – WebMD.” 8 Apr. 2018, https://www.webmd.com/a-to-z-guides/neutropenia-causes-symptoms-treatment. Accessed 23 Mar. 2020.
- “What are corticosteroids? – WebMD.” https://www.webmd.com/rheumatoid-arthritis/qa/what-are-corticosteroids. Accessed 23 Mar. 2020.
- “Definition of Prostaglandin – RxList.” https://www.rxlist.com/script/main/art.asp?articlekey=16461. Accessed 23 Mar. 2020.
- “COX-1 and COX-2 inhibitors. – NCBI.” https://www.ncbi.nlm.nih.gov/pubmed/11566042. Accessed 23 Mar. 2020.